How Doctors and Hospitals Can Help Defeat COVID-19 Vaccine Resistance and Misinformation
There's a recent rise in national optimism that says—maybe—we have turned the corner on the pandemic lockdown. Admittedly, it's been a tough year for nearly everyone, but miraculous vaccines and declining death rates have stirred newfound optimism.
But wait -- unfortunately, the COVID pandemic isn't over. Pandemic fatigue, misinformation, accelerated state re-openings, growing travel, and even politics all contribute to people prematurely abandoning safety measures, including mask-wearing and social distancing.
As a result, new coronavirus mutations, including the UK variant (B.1.1.7) have taken hold in the US and threaten to slow progress. Recent outbreaks nationwide are so troubling that last week CDC Director Dr. Rochelle Walensky implored us to "just hold on a little longer to get vaccinated when you can."
While Dr. Anthony Fauci doesn't predict a fourth wave as big as the previous three, he said, "It's kind of like a race between the potential for a surge and our ability to vaccinate as many people as we possibly can." At this juncture, politicians and experts agree that "Vaccinating a high percentage of the population against COVID-19 is a crucial part of the US strategy to curb the pandemic."
The Looming Vaccine Resistance Roadblock
Experts warn that vaccination resistance is now a significant challenge between today and 'the next normal.' According to the New England Journal of Medicine, "The potential for vaccines to interrupt US transmission of Covid-19…also depends on the willingness of a large proportion of the public to be vaccinated. Though there has been strong demand for the relatively small amount of vaccine available initially, maintaining interest in vaccination is a longer-term challenge."
According to recent polls, between 25% and 30% of Americans still say they probably or definitely will not get a vaccine. So while the present demand for the vaccines is greater than the supply, at a rate of 3 million shots delivered per day, that equation will likely soon reverse itself.
The anti-vaccine movement is widespread and complex. According to a March 2021 NPR/PBS/Marist survey, demographic groups who said they'd refuse a vaccine if offered include 49% of Republican men, 34% of white non-college graduates, 37% of Latinos, 37% of people under 45, 36% of those living in rural areas, 34% of men and 26% of women.
A Kaiser Health News poll conducted several weeks later shows somewhat more optimistic data but similarly found that among Republicans and white evangelical Christians, almost 30% maintain they will "definitely not" get a shot. According to Robert J. Blendon, a health policy scholar at Harvard, "We've never seen an epidemic that was polarized politically before."
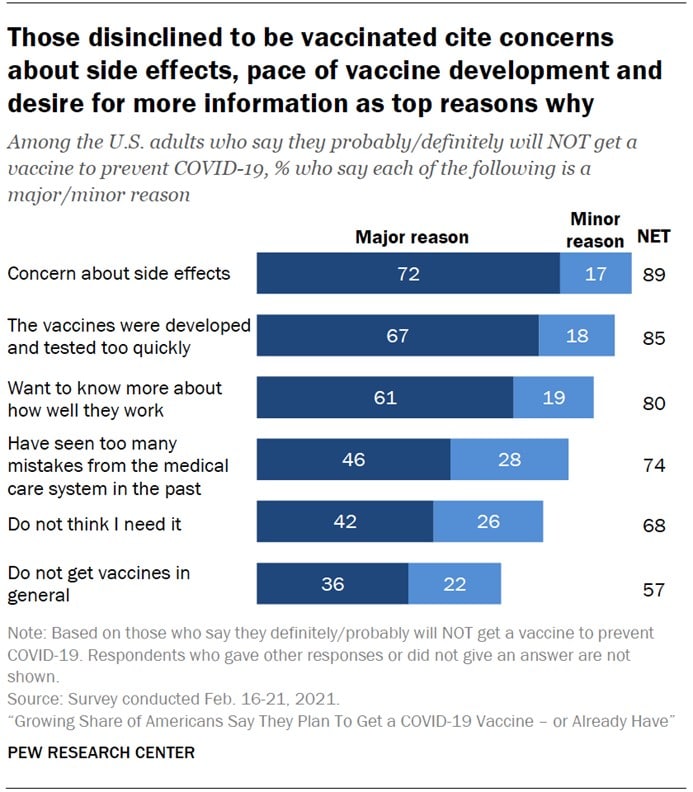
Beyond politics, there are several reasons why people say they will "definitely not" get a vaccine."
Finally, there remains an avalanche of COVID antivaxxer misinformation on social media, much of which can be traced to just twelve individuals.
Continued vaccine resistance could spell trouble for ending the pandemic as early as we'd all like. "Resisters are making it harder to achieve "herd immunity," the point at which the virus can no longer find new hosts to infect. That's when the pandemic will come to an end. Herd immunity against the coronavirus will require between 70% and 85% of the population to be vaccinated."
Why Healthcare Professionals Are Vital to Answering Resistance Issues
While the public only moderately trusts information provided by elected officials, government agencies such as the Food and Drug Administration, and medical scientists, doctors remain extraordinarily trusted. (NEJM) In fact, according to a recent NPR /Ipsos survey, 85% of Americans trust their personal doctor.
From a practical perspective and a marketing POV, doctors, hospitals, and other providers are ideal for educating patients on the COVID-19 vaccines. They are particularly ideal for communicating an effective and persuasive response to the "resistance challenge."
What's more, with the overarching need to depoliticize objections – and federal voices distrusted – it's critical for individuals to hear the vaccination message from their own local and trusted physician. Other reasons include:
- Throughout this pandemic, healthcare providers are recognized as the first line of defense and frontline heroes.
- Providers and hospitals have the most significant influence on individuals and respect in the community.
- Frontline healthcare providers represent authoritative information
- The doctor-patient connection has a foundation of close, personal trust.
- Doctors, hospitals and healthcare professionals are well-informed and have access to current and correct information.
- The provider-patient relationship is often well-established; rapport, empathy, support and trust have been created over time.
The NEJM agrees about the upside benefits of patient communications. "We believe that there is great potential for public willingness to receive Covid-19 vaccines but that effective public education and outreach are needed to maximize the proportion of the population that will do so quickly.
"We also believe that clinical physicians, rather than pharmaceutical companies, political leaders, or even medical scientists, should be at the fore of education and outreach strategies. Featuring clinicians in messaging is particularly important given that many people will not see their physician when making vaccination decisions."
Another Missing Link: Empower Hospitals and Medical Practices with Vaccine
"An MGMA survey finds that medical practices across the country are being left out of COVID-19 rollout efforts. The survey revealed a staggering 85% of independent practices and 45% of hospital or health system-owned practices actively seeking the COVID-19 vaccine for their patients report having obtained none to date."
MGMA and other publications are left wondering why the vaccine distribution left this gap in the communications plan. "Physician practices are uniquely situated to identify, reach out to, and vaccinate patients in their communities. As trusted providers in their communities, physicians can and should play a key role in vaccinating patients against COVID-19." What better opportunity for providers and patients to talk about vaccinations?
COVID-19 Vaccine Patient Education: How to Craft a Compelling and Convincing Message
Here are several tips, tactics and article resources to help communicate the importance of vaccination and, in particular, reach the reluctant segments of your target audience.
- Talk it up! Nothing beats word of mouth (WOM) marketing. Doctors, nurses, PAs and others all have unsurpassed credibility with patients. If you lead a health system or multi-location practice, think of innovative ways to inspire your providers and scale your WOM messaging.
- Social media. Utilize organic (free) and paid social media to get the word out. You will be doing a public service and position your hospital or practice as a leader in your community.
- Provider Videos. Even simple videos shot with smartphones can leverage the inherent trust patients have for their doctors.
- Email your patient base. Your patients are hungry for authoritative information about the COVID pandemic. They need your input now.
- Advertise. You can serve your community while building your brand by using precious advertising dollars to "get the word out."
- Promote vaccines in-office. Tried and true point-of-purchase (POP) tactics like posters, table tents, and flyers can help patients actively ask for advice.
- Keep current on COVID information. Keeping pace with the local, regional and national details can be challenging. The particulars change often, and it's vital to expect regular updates that help providers and the public.
- Identify your target audience segments. Understand the spectrum of public attitudes from "compliant" to "reluctant" to "outright rejection." These and every segment in between deserves a thoughtful and convincing response. Begin with the objections listed above and consider the most appealing benefits in reply.
- Consider demographics. Often political attitudes, age group, and other characteristics will influence attitudes and help shape the message.
- Capitalize on the influence of local celebrity spokespeople. One of my favorite marketing success stories is documented by Chip and Dan Health in Made to Stick. Their book includes details about how the Lone Star state convinced blue-collar, pickup truck driving "Bubbas" to stop littering on state highways. Rather than rely on fear, guilt, shame or cuddly owl characters, the "Don't Mess with Texas" campaign successfully stoked state pride and featured prominent Texas celebrities like Ed "Too Tall" Jones and Willy Nelson.
Similarly, most larger communities have recognized celebrity voices. They could be local heroes, sports figures, or hometown-person-makes-good. Hospitals and health systems can recruit well-known and credible individuals to help present the media's pro-vaccine message. Often these local celebrities will be pleased to participate, and their impact will be powerful.
The US Government Wants You to Join the Fight!
Finally, the federal government understands it cannot convince everyone to get vaccinated. Just last week, White House press secretary, Jen Psaki, admitted, "…we are not always the best messengers that — here, a Democratic administration — to communicate to everyone in public about the safety, the efficacy, and the importance of taking the vaccine."
Just now, a series of new public service and social media announcements are rolling out. These are in concert with broadcast messages from provider organizations, CDC announcements, state and local government spots – many with the national Ad Council's support.
To their credit, the government is also reaching out to trusted civic groups and community leaders and influencers – particularly those with conservative connections.
Nationwide, the New York Times reports: "The public awareness push includes 275 participating organizations that will speak to communities where skepticism of the coronavirus vaccine remains high." This national outreach network includes doctors, community and rural organizations, sports leagues, unions and religious groups.
WE CAN DO THIS: You Can Help…Informally or Not
At the grassroots level, the Health and Human Services Department encourages individuals and community groups to join the "We Can Do This" Community Corps education campaign. The website includes ads and other resources to help "increase vaccine confidence while reinforcing basic prevention measures."
Let's join forces as healthcare professionals to get the word out.
For more than a year, the Healthcare Success team and I have been working to support hospitals and providers in these difficult months. Here are several previous posts that contain helpful guidance:
How to Create an Effective COVID-19 Vaccine Communication Strategy for Your Patients
[Podcast] How to Adjust Your Creative Strategies in Response to the COVID-19 Pandemic
How Are Healthcare Consumers Responding to COVID/the Coronavirus Pandemic?
Related Articles:
How to Create an Effective COVID-19 Vaccine Communication Strategy for Your Patients
Best of 2021: 14 Insights from Healthcare Marketing Experts
Is COVID the Rx for the Pharmaceutical Industry's Reputation?
COVID-19: Healthcare Marketing Adjustments To Make in Response to Coronavirus